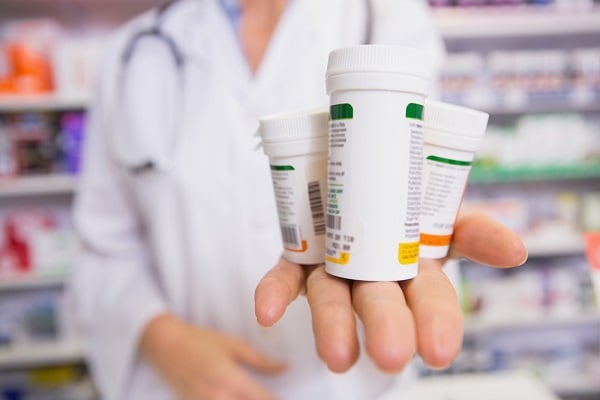
 For years, small pharmacy owners have been complaining that PBMs have been shortchanging them, cutting to unsustainable amounts the reimbursement they get. (Photo: Shutterstock)
For years, small pharmacy owners have been complaining that PBMs have been shortchanging them, cutting to unsustainable amounts the reimbursement they get. (Photo: Shutterstock)
Pharmacy-benefit managers are taking increasingly large markups on generic drugs in New York, according to an analysis of Medicaid prescriptions at independent pharmacies in the state.
In Medicaid, private insurers are paid by the state to cover low-income citizens. The insurers in turn usually contract with pharmacy-benefit managers, or PBMs, paying them to provide drug coverage. PBMs run by CVS Health Corp., Cigna Corp. and UnitedHealth Group Inc. then bill insurers for coverage, and reimburse pharmacies for drugs.
Recommended For You
Complete your profile to continue reading and get FREE access to BenefitsPRO, part of your ALM digital membership.
Your access to unlimited BenefitsPRO content isn’t changing.
Once you are an ALM digital member, you’ll receive:
- Breaking benefits news and analysis, on-site and via our newsletters and custom alerts
- Educational webcasts, white papers, and ebooks from industry thought leaders
- Critical converage of the property casualty insurance and financial advisory markets on our other ALM sites, PropertyCasualty360 and ThinkAdvisor
Already have an account? Sign In Now
© 2025 ALM Global, LLC, All Rights Reserved. Request academic re-use from www.copyright.com. All other uses, submit a request to [email protected]. For more information visit Asset & Logo Licensing.