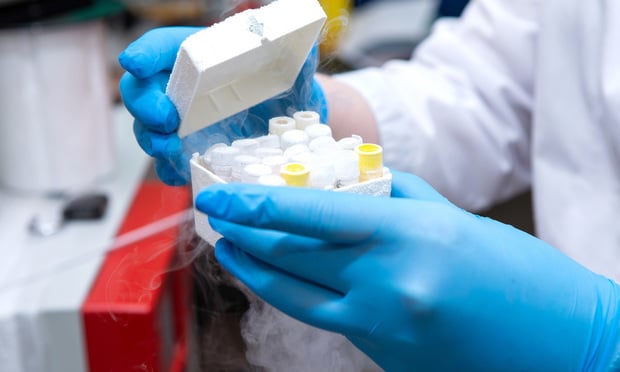
Lawmakers and patient advocacy groups have been pushing for legal changes to reduce surprise billing. (Photo: Shutterstock)
Lawmakers and patient advocacy groups have been pushing for legal changes to reduce surprise billing. (Photo: Shutterstock)
Out-of-network billing increased sharply between 2010 and 2016, according to a new study released by JAMA Internal Medicine.
In an analysis of 13.5 million emergency department admissions, researchers at Stanford found that patients were billed for services outside of their insurance network 42.8 percent of the time in 2016, up from only 32.3 percent six years earlier.
Recommended For You
Complete your profile to continue reading and get FREE access to BenefitsPRO, part of your ALM digital membership.
Your access to unlimited BenefitsPRO content isn’t changing.
Once you are an ALM digital member, you’ll receive:
- Breaking benefits news and analysis, on-site and via our newsletters and custom alerts
- Educational webcasts, white papers, and ebooks from industry thought leaders
- Critical converage of the property casualty insurance and financial advisory markets on our other ALM sites, PropertyCasualty360 and ThinkAdvisor
Already have an account? Sign In Now
© 2025 ALM Global, LLC, All Rights Reserved. Request academic re-use from www.copyright.com. All other uses, submit a request to [email protected]. For more information visit Asset & Logo Licensing.